Have you been suffering from persistent shoulder pain that’s been affecting your daily activities? If so, you’re not alone. Calcific tendonitis, a common orthopaedic condition, can be a source of discomfort and disruption in your life. At the Sydney Orthopaedic Surgeon Clinic, we understand the impact that calcific tendonitis can have on your well-being, and we’re here to provide the help and expertise you need.
Leading our team is Dr Stuart Kirkham, a highly experienced and well-respected orthopaedic surgeon with over 25 years of expertise in musculoskeletal conditions, including calcific tendonitis. His dedication to personalised care ensures that your unique needs are met with precision and compassion. The crucial difference of Dr Kirkham’s care is that he doesn’t believe in one-size-fits-all solutions. Instead, Dr Kirkham tailors treatments to your specific situation, whether you’re grappling with mild discomfort or facing a more severe case demanding surgical intervention.
His holistic approach begins with a thorough diagnosis and examination before combining cutting-edge non-surgical treatments with advanced surgical options, when necessary, like needle lavage and arthroscopic surgery. Our mission is clear: to alleviate your pain, restore your freedom of movement, and elevate your quality of life. If calcific tendonitis is causing you concern, please don’t hesitate to reach out to Dr Kirkham and his experienced team. With five conveniently located clinic spread across the city of Sydney, Dr Kirkham is committed to helping the whole community.
Take that crucial first step towards a pain-free, active, and fulfilling life by scheduling a consultation with Dr Kirkham today. Your journey to recovery starts here, and Dr Kirkham is ready to guide you every step of the way.
Anatomy Affected by Calcific Tendonitis
In simple terms, calcific tendonitis is the formation of calcium deposits within the tendons. These deposits can range in size from tiny grains to larger, more troublesome formations which often occurring in the rotator cuff tendons of the shoulder. But what are tendons, and what is the rotator cuff?
Tendons are the tough, fibrous tissues that connect muscles to bones. In the context of calcific tendonitis, the focus is primarily on those tendons within the shoulder joint. These tendons are crucial for shoulder movement and stability, and there are four main tendons within the shoulder that collectively are known as the rotator cuff. They consist of the supraspinatus, infraspinatus, teres minor, and subscapularis tendons, and they work together to allow you to lift your arm, rotate it, and perform various daily activities.
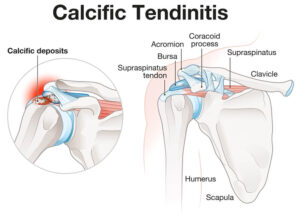
Tendons serve as connectors, transmitting the force generated by muscles to the bones they’re attached to. They are essential for maintaining joint stability and facilitating smooth movement. But when calcium deposits form within the tendons, they can lead to inflammation, pain, and reduced mobility. The presence of these deposits can weaken the tendons, making them more susceptible to injury and therefore limiting the function of the shoulder and arm as a whole. As a result, you may experience persistent pain, stiffness, and difficulty performing everyday tasks that require shoulder movement.
To ensure you receive the best possible care for your calcific tendonitis, don’t hesitate to contact Dr Kirkham for a consultation today. His commitment to personalized care and in-depth assessment ensures that you’ll receive a precise diagnosis and a customised plan for your calcific tendonitis recovery. Embark on the journey to a more comfortable daily life – reach out to Dr Kirkham now and take the first step toward addressing your calcific tendonitis.
Causes and Risk Factors for Calcific Tendonitis
Though it is a common condition, calcific tendonitis is complex, and while its causes are known, there are question marks over its inherent risk factors.
The cause of these calcium deposits can broadly be categorised into two types: degenerative calcification and reactive calcification. Degenerative calcification occurs gradually over time, often due to age and wear and tear on the tendons. This type is more common in individuals between the ages of 40 and 60, and it can affect both men and women. However, women are slightly more predisposed to this condition than men.
Reactive calcification, on the other hand, is characterised by a more abrupt and painful onset. It is not as age-dependent and can affect individuals of varying age groups. The exact trigger for reactive calcification is not always clear but may be related to metabolic factors.
Calcific tendonitis also tends to progress through three distinct stages. In the pre-calcific stage, individuals may experience pain during movement, and their range of motion may become limited. At the cellular level, changes are occurring within the affected area, setting the stage for calcification.
The calcific stage sees the release of calcium from cells, forming deposits within the tendon. This stage can be particularly uncomfortable and may cause significant pain and stiffness.
Finally, in the post-calcific stage, the body begins to resorb the calcium deposits, gradually replacing them with healthy tissue. During this stage, there’s a notable improvement in the range of motion, and the discomfort starts to subside.
In addition to age-related factors, lifestyle and occupational factors can contribute to the development of calcific tendonitis. Unlike some orthopaedic conditions associated with specific activities, calcific tendonitis can affect individuals from all walks of life, making it a condition with no particular occupational predisposition. Genetics may also play a role in susceptibility to calcific tendonitis, and certain medical conditions, such as diabetes and thyroid disorders, have been linked to an increased risk of calcific tendonitis.
Understanding the multifaceted nature of calcific tendonitis, its various stages, and the factors contributing to its development is essential for effective diagnosis and treatment. If you’re experiencing symptoms or have concerns about calcific tendonitis, consult with Dr Kirkham for a comprehensive evaluation and tailored treatment plan today.
Symptoms and Identification of Calcific Tendonitis
The onset of calcific tendonitis is often accompanied by a range of symptoms, with the most common including persistent shoulder pain, stiffness, and a noticeable reduction in your range of motion. You may find it challenging to perform everyday tasks that involve raising your arm or reaching overhead. Additionally, tenderness in the rotator cuff area can often be felt, especially when pressure is applied.
To identify signs of calcific tendonitis at home, pay attention to the pain’s persistence and intensity. If you experience ongoing discomfort that doesn’t seem to improve with rest or over-the-counter pain medications, it could be a potential indicator. Additionally, if you notice a decreased ability to move your shoulder or perform activities you could previously do without issue, this may also be a sign of calcific tendonitis.
However, it’s important to note that a definitive diagnosis should always be obtained from a medical professional. If you are experiencing these symptoms, it’s advisable to seek medical advice promptly. Delaying a consultation could prolong your discomfort and potentially lead to complications.
If you have been experiencing persistent shoulder pain, weakness, limited range of motion, or difficulty with everyday activities, Dr Kirkham can assist you with a comprehensive identification process that ensures an accurate and timely diagnosis. His expertise means that you can expect an examination that goes beyond simple tests and physical exams and uses a combination of expertise and analysis along with a range of imaging and diagnosis techniques that accurately seek out the root cause of your pain. Don’t let the discomfort linger—take the proactive step towards relief and recovery by scheduling a consultation with Dr Kirkham today.
Diagnosis and Imaging of Calcific Tendonitis
Diagnosing calcific tendonitis involves a comprehensive assessment to pinpoint the condition accurately. Under Dr Kirkham’s care, the diagnostic process typically begins with a physical examination where Dr Kirkham assesses your shoulder’s range of motion, palpates the affected area for tenderness, and gathers information about your symptoms and medical history.
Following the physical examination, the next step in the process is utilising imaging techniques. X-rays are typically the initial choice because they can provide a very clear visualisation of calcified deposits within the tendons. If the X-ray reveals significant calcification, it can strongly support the diagnosis of calcific tendonitis.
However, in cases where X-rays do not provide a clear diagnosis or when there is a suspicion of other shoulder pathologies, additional imaging may be necessary. Ultrasound is a valuable tool for assessing soft tissue structures, including the tendons and any associated calcium deposits. Ultrasound can offer real-time images and dynamic assessment of the shoulder.
For more complex cases or when a higher level of detail is needed, MRI scans may be used to provide a detailed view of the soft tissues and differentiate calcific tendonitis from other shoulder conditions, such as rotator cuff tears. Differentiating calcific tendonitis from other shoulder pathologies is crucial for providing the appropriate treatment.
If you’re concerned that you may have been experiencing the symptoms of calcific tendonitis, or if you have a family history of these conditions, it’s crucial to seek expert medical advice for a thorough diagnosis and for your own peace of mind. Dr Kirkham and the team at the Sydney Orthopaedic Surgeon Clinic have extensive experience in diagnosing and treating calcific tendonitis, and by seeking their specialised care, you can set yourself on the road to recovery.
Treatment Options for Calcific Tendonitis
When it comes to treating calcific tendonitis, various options are available, ranging from non-surgical interventions to more advanced procedures. The choice of treatment depends on the severity of your condition and your specific needs.
Non-surgical treatments are often the first line of defence against calcific tendonitis. These include medication to manage pain and inflammation, as well as physiotherapy to improve shoulder strength and mobility. Shock wave therapy is another non-invasive option.
Extracorporeal Shockwave Therapy (ESWT) delivers shock waves to the affected tendons, reducing pain and stimulating the healing process. Similarly, Radial Shockwave Therapy (RSWT) also focuses on pain reduction and healing but uses a different technique to generate shockwaves. Therapeutic ultrasound is yet another non-surgical approach, and it involves directing high-frequency sound waves to the target area, helping break down the troublesome calcium deposits.
In some cases when non-surgical treatments aren’t effective or if calcific tendonitis is particularly severe, more invasive options may be considered. Needle lavage or decompression is a procedure where the calcium deposits are flushed out using a needle. It can be appropriate when other methods have failed to provide relief.
Alternatively, Dr Kirkham may instead recommend cortisone injections to alleviate pain and inflammation. This will only be effective temporarily, but as cortisone is extremely strong, it should provide relief for several months by reducing inflammation and swelling.
For cases where non-surgical treatments have proven insufficient, or if the calcific deposits are causing significant discomfort, Dr Kirkham may utilise keyhole surgery or arthroscopic decompression may be recommended. This minimally invasive surgical approach allows for the removal of the calcium deposits and any damaged tissue, providing relief and promoting healing.
The choice of treatment is not one-size-fits-all and should be tailored to your unique condition and needs. Dr Kirkham specialises in the treatment of calcific tendonitis and will work closely with you to determine the most appropriate course of action. Whether through non-surgical interventions or advanced procedures, the goal is to alleviate your pain and restore your shoulder’s functionality. Don’t hesitate to seek Dr Kirkham’s expert advice and explore the range of treatment options available to you for effective relief and recovery.
Prevention and Aftercare for Calcific Tendonitis
While calcific tendonitis cannot always be completely prevented explicitly, there are proactive measures you can take to reduce the risk of recurrence and ensure a smoother recovery. First and foremost, if you experience any shoulder pain or discomfort, it’s essential not to engage in strenuous activities until you’ve had it evaluated by a healthcare provider. Ignoring early warning signs can exacerbate the condition.
Furthermore, incorporating specific exercises into your routine can help strengthen the shoulder muscles and improve overall joint stability. Dr Kirkham can recommend tailored exercises to address your individual needs. Lifestyle adjustments may also be necessary to avoid activities that could strain the shoulder or contribute to the recurrence of calcific tendonitis.
Once you’ve undergone treatment for calcific tendonitis, it’s crucial to follow a post-treatment care plan to minimise the risk of recurrence. This may include continued exercise, medication management, and lifestyle modifications. Consistency in adhering to these recommendations can significantly improve your chances of a successful recovery.
The importance of following a care plan developed by healthcare professionals cannot be overstated. These plans are designed to address your specific condition and needs, ensuring that you receive the most effective care possible. Deviating from the recommended course of action could hinder your recovery and increase the risk of complications.
If you’ve been dealing with calcific tendonitis and haven’t received an effective aftercare plan, don’t hesitate to reach out to Dr Kirkham for specialised care to support your recovery journey. Your shoulder health and well-being are our top priorities, and Dr Kirkham is committed to ensuring each of his patients experiences a smooth recovery before returning to their daily activities with confidence.
The Recovery Process from Calcific Tendonitis
Recovery from calcific tendonitis, weather through surgical intervention or non-surgical treatments, involves several essential components to ensure a smooth and effective healing process.
In most cases where surgery is required, the typical recovery timelines for calcific tendonitis is approximately six weeks. During this period, it’s common to wear a sling to immobilise the shoulder joint and prevent excessive movement that could hinder the healing process. The use of a sling also helps to protect the surgical site and allows the tendons to repair and recover.
Rehabilitation exercises and physical therapy play a vital role in the recovery process. Starting early and gradually increasing movement and strength is essential. Following a surgical procedure, a physiotherapist will provide a tailored program of strengthening and stretching exercises to be performed both during therapy sessions and at home. These exercises are designed to rebuild muscle strength and flexibility, restore normal range of motion, and improve overall shoulder function.
Even if surgery was not necessary and non-surgical treatments were pursued, Dr Kirkham still recommends his patients to attend physiotherapy sessions in many instances. Strengthening the rotator cuff muscles can reduce pressure on the calcium deposits within the tendon, and this can help facilitate their resorption and overall recovery. Physiotherapy sessions are invaluable in guiding you through the appropriate exercises and ensuring you perform them correctly.
The recovery process for calcific tendonitis does require patience and resilience, but with the help of Dr Kirkham, it is entirely possible to regain shoulder function and escape from discomfort in a matter of weeks. Whether you’ve undergone surgery or opted for more conservative measures, Dr Kirkham is always available to assist you in your journey towards restoring full shoulder function and enjoying a pain-free daily experience.
Possible Complications of Calcific Tendonitis
While treating calcific tendonitis can lead to significant improvement, it’s essential to be aware of potential complications that may arise during the recovery process. Some individuals may experience persistent pain and discomfort even after treatment. This can be due to residual inflammation or complications related to the procedure.
Alternatively, some patients may experience adhesive capsulitis, which is also known as a “frozen shoulder”. This can develop as a complication of calcific tendonitis. It involves the thickening and tightening of the shoulder joint capsule, leading to restricted movement and pain. In some cases, the calcification process may weaken the tendons, increasing the risk of rotator cuff tears. These tears can result in pain and further loss of shoulder function.
Greater Tuberosity Osteolysis may also be experienced in some cases. This condition involves the erosion of the greater tuberosity of the humerus bone in the shoulder. It can occur as a result of long-term calcific tendonitis or surgical interventions. In rare cases, calcific tendonitis can also progress to ossifying tendinitis, where calcium deposits turn into bone within the tendon. This can lead to severe pain and reduced mobility.
It’s also important to remember that any surgical procedure, including those for calcific tendonitis, carries inherent risks. These risks may include infection, bleeding, adverse reactions to anaesthesia, and, in rare cases, damage to nearby structures. Dr Kirkham always discusses these potential risks before all procedures, but you can take comfort in the fact that Dr Kirkham has decades of training, experience and research guiding his work. His intimate understanding of the relevant procedures and the condition itself means that you remain in the hands of a highly trained industry expert at all times.
Are You Concerned About Calcific Tendonitis?
Discovering that you have calcific tendonitis, whether it causes significant discomfort or not, can be an emotionally challenging experience. The uncertainty that comes with such a diagnosis can be distressing, but with Dr Kirkham’s assistance, you’re never alone in this journey.
Dr Kirkham is dedicated to providing empathetic and comprehensive care to each of his patients, and he understands how difficult the conditions he treats can be. He prioritises your well-being and comfort throughout the entire process, ensuring you receive the information and support you need to navigate this condition.
During your initial consultation with Dr Kirkham, you can anticipate a thorough assessment and a detailed discussion of your condition. This consultation will provide you with valuable insights into your diagnosis, treatment options, and what to expect throughout your care journey.
If you have concerns about calcific tendonitis, please don’t hesitate to reach out. Contact us today to schedule a consultation with Dr Kirkham and take the first step towards expert care, enhanced health, and peace of mind. Your health and comfort are our primary priorities, and Dr Kirkham is here to provide dedicated support every step of the way.
FAQs
1. What is calcific tendonitis and why does it occur?
Calcific tendonitis is a condition characterized by the accumulation of calcium deposits within a tendon, most commonly affecting the rotator cuff tendons in the shoulder. The exact cause of calcific tendonitis is not always clear, but it typically results from a combination of factors. Age-related wear and tear on the tendons, genetic predisposition, and metabolic factors can contribute to its development. These calcium deposits form within the tendon, leading to pain, stiffness, and reduced range of motion in the affected shoulder.
2. How is calcific tendonitis diagnosed?
The diagnosis of calcific tendonitis involves a comprehensive evaluation by a healthcare professional. It typically begins with a physical examination, where the provider assesses the range of motion, palpates the affected area for tenderness, and gathers information about the patient’s symptoms and medical history. Imaging techniques such as X-rays, ultrasound, and MRI are often used to confirm the diagnosis. X-rays can reveal the presence and extent of calcium deposits, while ultrasound and MRI provide detailed images of the soft tissues and can help differentiate calcific tendonitis from other shoulder pathologies.
3. Are there any home remedies for calcific tendonitis?
While calcific tendonitis should be evaluated and treated by a healthcare professional, there are some self-care measures that individuals can consider. These include rest and avoiding activities that exacerbate symptoms, applying ice to the affected area to reduce inflammation, and over-the-counter pain medications for pain relief. Gentle stretching exercises recommended by a healthcare provider can also help maintain range of motion. However, it’s essential to consult with a medical professional to determine the most appropriate treatment plan for your specific condition.
4. Can calcific tendonitis be completely cured?
The outcome of calcific tendonitis treatment varies from person to person. In many cases, with the right treatment and rehabilitation, individuals can experience significant relief from symptoms and regain full shoulder function. However, it’s important to note that a complete and permanent “cure” may not always be possible, especially in more advanced cases. The goal of treatment is often focused on managing symptoms, reducing calcium deposits, and improving shoulder function to enhance the individual’s quality of life.
5. How long does it take to recover from calcific tendonitis?
The duration of recovery from calcific tendonitis can vary depending on several factors, including the severity of the condition, the chosen treatment approach, and individual patient characteristics. In general, non-surgical treatments may lead to improvement within a few weeks to a few months, while surgical interventions may have longer recovery periods, often taking several months to achieve optimal results. Physical therapy and rehabilitation exercises are typically a crucial part of the recovery process, helping to regain strength and mobility. It’s essential to work closely with a healthcare provider to establish realistic expectations and monitor progress throughout the recovery journey.
References
- Cleveland Clinic (Calcific Tendonitis: Symptoms, Causes, & Treatment)
- Mayo Clinic (Sports-Medicine-Physician-Dr-Shapiro)
- UVA Health (Shoulder Calcific Tendonitis)


