If you’ve been living with persistent pain and limited mobility caused by shoulder arthritis, relief may be closer than you think. Welcome to the informative world of Arthroplasty for Shoulder Arthritis—a ground-breaking surgical solution that can transform your life and restore your shoulder’s functionality.
Shoulder arthritis can severely impact your daily activities, hindering your ability to enjoy life to the fullest. However, Dr Kirkham and his team are here to provide expert care and comprehensive solutions. Arthroplasty, a surgical procedure that replaces the damaged joint with an artificial one, can alleviate pain, restore mobility, and improve overall shoulder function. Dr Kirkham’s personalised approach ensures that each patient receives individualised care and a tailored treatment plan.
If you find yourself grappling with shoulder arthritis, take solace in the fact that relief is within reach. At the Sydney Orthopaedic Surgeon Clinic, our dedicated team is committed to assisting you on your journey to regain optimal shoulder function. Please don’t hesitate to reach out to us to schedule a consultation with Dr Kirkham, who will collaborate closely with you to identify the most suitable solution for your specific needs. Together, let’s strive to restore your shoulder’s mobility and empower you to engage in the activities you cherish.
Anatomy
The shoulder is one of the most mobile joints in the body, allowing for a huge range of motion. It consists of several key components that work together to facilitate movement and provide stability. At the heart of the shoulder joint is the humerus, the upper arm bone that fits into the shallow socket of the scapula, known as the glenoid. This ball-and-socket structure allows for the shoulder’s remarkable flexibility.
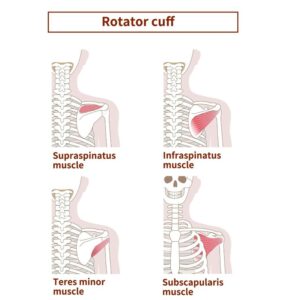
The role of the shoulder’s components is integral to its overall functionality. The rotator cuff, a group of tendons and muscles, is crucial in stabilising the joint and facilitating various arm movements. It consists of four muscles: the supraspinatus, infraspinatus, teres minor, and subscapularis. Each of these muscles works together to ensure the proper alignment and movement of the shoulder joint.
Arthritis can significantly affect the shoulder’s anatomy and overall function. Shoulder arthritis is the inflammation and deterioration of the joint’s cartilage, leading to pain, stiffness, and limited range of motion. The smooth surface of the cartilage becomes rough and eroded, causing bone-on-bone contact within the joint. This not only impairs movement but also triggers pain and discomfort.
Understanding the relationship between arthritis and shoulder anatomy is essential in guiding treatment decisions. Depending on the specific type and severity of arthritis, different components of the shoulder may be affected. For instance, in osteoarthritis, the deterioration of cartilage is the primary concern, while rheumatoid arthritis involves an autoimmune response that affects multiple structures within the joint.
Ensuring the stability of the shoulder joint is of utmost importance, especially for individuals who have undergone arthroplasty for shoulder arthritis. Dr Kirkham and his team specialise in providing specialised care to manage and prevent shoulder arthritis. With their expertise in shoulder arthroplasty and post-operative care, you can rest assured that your shoulder’s well-being will be resorted by a highly experienced and well-respected professional.
Causes and Risk Factors
Shoulder arthritis can arise from various causes, each with its own impact on the joint’s health and function. One common cause is osteoarthritis, which occurs due to the natural wear and tear of the joint over time. This degenerative condition gradually erodes the protective cartilage, leading to bone-on-bone contact, inflammation, and discomfort. Another prevalent cause is rheumatoid arthritis, an autoimmune disorder that triggers inflammation and damages the joint tissues.
Several factors can increase the risk of developing arthritis in the shoulder. Age is a significant factor, as the likelihood of developing shoulder arthritis increases with advancing years. The wear and tear on the joint accumulate over time, contributing to the degenerative changes.

Genetic factors also play a role, as certain individuals may have a predisposition to develop arthritis due to inherited traits. Additionally, lifestyle factors, such as occupations or activities that involve repetitive overhead motions or heavy lifting, can contribute to shoulder arthritis by placing excessive stress on the joint.
A range of alternative risk factors can also influence the development of shoulder arthritis. Previous injuries, such as fractures or dislocations, can disrupt the shoulder joint’s normal anatomy and contribute to the onset of arthritis. Certain medical conditions, including obesity and metabolic disorders, may increase the risk of joint deterioration. Inflammatory diseases, such as gout or lupus, can also affect the shoulder joint and contribute to arthritis.
Understanding these causes and risk factors is essential in recognising the potential for shoulder arthritis and adopting preventive measures. Dr Kirkham always delivers exceptional patient care, and this extends to educating patients about these risk factors and providing guidance on lifestyle modifications to reduce the likelihood of developing or worsening shoulder arthritis. By addressing these factors, individuals can proactively protect their shoulder health and maintain optimal joint function for years to come.
Symptoms and Identification
Shoulder arthritis manifests through a range of symptoms that can significantly impact an individual’s quality of life. Common symptoms include persistent shoulder pain, which may worsen with movement or at night, limiting one’s ability to sleep comfortably. Stiffness and decreased range of motion in the shoulder joint are also prevalent, making it challenging to perform daily activities such as reaching or lifting objects. The affected shoulder may feel weak, and individuals may experience a grinding sensation or audible clicking sounds during movement.
Identifying shoulder arthritis initially relies on recognising these characteristic symptoms. If you find yourself consistently experiencing shoulder pain that doesn’t subside with rest or over-the-counter pain medications, it may be an indication of an underlying issue.
Stiffness and limited range of motion that persist for an extended period, hindering your ability to perform routine tasks, should also raise concern. Additionally, if you notice a gradual decline in shoulder function and increasing difficulty in maintaining an active lifestyle, it may be time to consider seeking medical help.
It is essential to consult a healthcare professional when symptoms interfere with your daily activities or when the pain becomes unbearable, impacting your overall well-being. Seeking medical help promptly is crucial to receive an accurate diagnosis and develop an appropriate treatment plan. Dr Kirkham and his team at the Sydney Orthopaedic Surgeon Clinic specialise in diagnosing and managing shoulder arthritis. Through a thorough examination and evaluation of your symptoms, they can provide an accurate diagnosis and recommend the most suitable treatment options to alleviate your pain, restore shoulder function, and enhance your quality of life.
Diagnosis and Imaging
Dr Stuart Kirkham employs various examination methods to diagnose shoulder arthritis accurately. He begins with a comprehensive medical history review, discussing your symptoms, their duration, and any previous injuries or conditions that may contribute to shoulder arthritis. During a physical examination, he will assess your shoulder’s range of motion, stability, and any signs of inflammation or tenderness.
To further aid in the diagnosis, imaging methods are utilised. Different types of imaging, such as X-rays, MRI scans, and CT scans, play a crucial role in evaluating the condition of the shoulder joint.
X-rays provide detailed images of the bones and can help identify joint degeneration, bone spurs, or other abnormalities associated with arthritis. MRI scans utilise powerful magnets and radio waves to generate high-resolution images, allowing for a more detailed view of the soft tissues, including the cartilage and tendons. CT scans provide cross-sectional images that can aid in detecting bone abnormalities and assessing the joint’s overall structure.
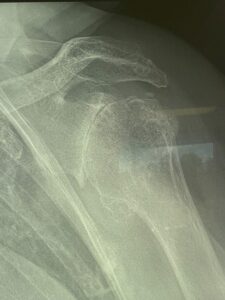
Figure 1 – Osteoarthritic Shoulder Joint
Early and accurate diagnosis of shoulder arthritis is vital for several reasons. Firstly, it allows for timely intervention and appropriate treatment planning. Early detection enables Dr Kirkham to recommend conservative approaches, such as medication, physical therapy, or lifestyle modifications, to manage symptoms effectively and potentially slow down the progression of the disease. Additionally, an accurate diagnosis ensures that the chosen treatment approach is tailored specifically to your condition, maximising the likelihood of successful outcomes.
Moreover, an early and accurate diagnosis can prevent potential complications. Untreated or improperly managed shoulder arthritis can lead to increased pain, loss of function, and further deterioration of the joint. By identifying the condition promptly, Dr Kirkham can implement suitable treatment strategies to minimise discomfort, improve shoulder function, and enhance your overall quality of life.
By using a combination of thorough examinations and advanced imaging techniques, Dr Kirkham aims to achieve early and accurate diagnoses of shoulder arthritis. This approach enables him to provide individually created treatment plans and interventions that address each patient’s unique needs. Contact the Sydney Orthopaedic Surgeon Clinic to schedule a consultation and benefit from Dr Kirkham’s expertise in diagnosing and managing shoulder arthritis effectively.
Treatment Options
When it comes to treating shoulder arthritis, several options are available, each tailored to address the unique needs of patients. Let’s explore the main treatment modalities in detail.
Standard (Total) Arthroplasty
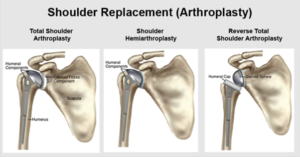
One common surgical approach is standard arthroplasty, which involves replacing the damaged parts of the shoulder joint. In this procedure, the ball (humeral head) is replaced with a prosthetic ball, while the socket (glenoid) is replaced with an artificial socket.
Typically, the humeral component is made of titanium and chrome cobalt, sometimes utilising pyrocarbon. The glenoid side is commonly composed of highly engineered and tested polyethylene, a specialised plastic. Standard arthroplasty is advantageous as it preserves the rotator cuff tendons, allowing for improved shoulder stability and function.
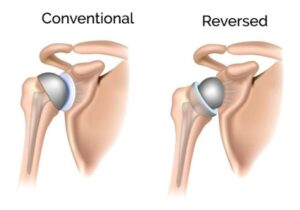
Reversed Arthroplasty
Another surgical option is reversed arthroplasty. In this procedure, the ball (humeral head) is replaced with a socket, and the socket (glenoid) is replaced with a ball. The humeral component is typically made of titanium and polyethylene, while the glenoid component consists of titanium and chrome cobalt.
Reversed arthroplasty is particularly beneficial for patients with irreparable rotator cuff tendons. The ingenious design of this procedure allows the shoulder to move effectively, compensating for the lack of rotator cuff support.
Hemiarthroplasty
Hemiarthroplasty is often employed for fractures of the humerus and in younger patients. In this procedure, only the humeral head is replaced, while the glenoid remains intact. Hemiarthroplasty may utilise pyrocarbon heads, providing an alternative material option.
Dr Kirkham has even designed and patented a specific hemiarthroplasty for fractures, although it is currently in the prototype stage and not yet in clinical use. He envisions its future incorporation into clinical practice to enhance treatment options for patients.
The choice of treatment depends on various factors, including the patient’s condition, age, and individual circumstances. Dr Kirkham will thoroughly assess your case and recommend the most suitable option to address your shoulder arthritis and optimise your long-term outcomes. Whether it’s standard arthroplasty, reversed arthroplasty, or hemiarthroplasty, Dr Kirkham’s expertise ensures that you receive top-quality care and receive the best possible treatment for your specific needs.
Prevention and Aftercare
Preventative Measures
Preventing the onset or progression of shoulder arthritis is crucial for maintaining optimal shoulder health. While some risk factors like age and genetics are beyond our control, there are measures we can take to minimise the likelihood of developing or worsening shoulder arthritis. Maintaining a healthy weight is essential, as excess weight puts additional strain on the joints, including the shoulders.
Regular exercise, including strength training and stretching exercises, can help keep the shoulder joint strong and flexible. It’s also important to avoid repetitive overhead motions or activities that place excessive stress on the shoulder, as these can contribute to joint wear and tear. Lastly, practising good posture and using proper body mechanics when lifting heavy objects can help prevent unnecessary strain on the shoulders.
Aftercare
After undergoing arthroplasty, proper aftercare is vital to ensure optimal recovery and long-term success. Following the surgical procedure, Dr Kirkham will provide you with specific guidelines tailored to your needs. These may include wound care instructions, pain management strategies, and recommendations for physical therapy.
Adhering to these guidelines is crucial for a smooth recovery and the best possible outcome. Physical therapy plays a significant role in rehabilitation, helping to restore strength, range of motion, and stability in the shoulder joint. It is important to actively participate in the prescribed exercises and attend therapy sessions as scheduled.
Additionally, making certain lifestyle changes can contribute to effective aftercare. Avoiding smoking is highly recommended, as it can hinder the healing process and increase the risk of complications. It’s also crucial to maintain a healthy lifestyle, including a well-balanced diet rich in nutrients that support bone health and overall well-being. Staying hydrated and getting sufficient rest and sleep are equally important for the body’s healing processes.
Dr Kirkham will provide you with comprehensive guidance on aftercare, ensuring that you have all the tools and resources necessary for a successful recovery. By following these tips, embracing healthy habits, and actively participating in your rehabilitation, you can expect to see pleasing results from your arthroplasty procedure and enjoy a pain-free, functional shoulder for years to come.
The Recovery Process
The recovery process following shoulder arthroplasty involves several key aspects that contribute to successful rehabilitation and restoration of shoulder function. Understanding what to expect during the recovery process can help you navigate this period with confidence and optimise your outcomes.
After the surgery, you will typically spend a short period of time in the hospital for monitoring and initial recovery. Pain management strategies will be in place to ensure your comfort. Once discharged, you will continue your recovery at home, under Dr Kirkham’s guidance. It’s normal to experience some discomfort and swelling during the initial stages of recovery, which can be managed with prescribed medications and proper rest.
The recovery process can be divided into different phases, each with its own goals and expected timelines. Initially, the focus is on wound healing and pain management. As the healing progresses, you will gradually begin physical therapy to restore shoulder mobility and strength. Physical therapy plays a crucial role in the recovery process, with exercises and targeted movements designed to improve the range of motion, strengthen the surrounding muscles, and enhance stability in the shoulder joint.
The duration of the recovery process can vary depending on various factors, including the extent of the surgery, individual healing abilities, and adherence to rehabilitation protocols. Typically, it takes several weeks to regain a reasonable range of motion in the shoulder. Over time, as the healing continues and the shoulder strengthens, you can gradually increase the intensity and complexity of the exercises.
Regular follow-up appointments with Dr Kirkham will be essential in monitoring your progress and making any necessary adjustments to your recovery plan. It’s important to communicate any concerns or difficulties you may encounter during the recovery process, as Dr Kirkham is dedicated to supporting you every step of the way.
Possible Complications
While shoulder arthroplasty is generally a safe and effective procedure, like any surgery, it carries potential risks and complications. It’s important to be aware of these possibilities to make informed decisions and manage expectations.
Some potential complications related to shoulder arthroplasty include infection, blood clots, nerve injury, implant loosening or failure, stiffness, and persistent pain. Infections can occur at the surgical site and may require antibiotic treatment. Blood clots can form in the veins of the arm or shoulder, necessitating preventive measures and monitoring.
Nerve injury is a rare but possible complication that can result in temporary or permanent loss of sensation or movement. Implant-related issues, such as loosening or failure, may require revision surgery. Stiffness and persistent pain can occur during the recovery process and may require additional interventions or physical therapy.
Dr Kirkham and his experienced team take every precaution to manage and mitigate these risks. They adhere to strict protocols to minimise the risk of infection, such as maintaining a sterile surgical environment and prescribing antibiotics as needed. To prevent blood clots, appropriate preventive measures are implemented, including early mobilisation and the use of compression stockings or blood-thinning medications.
Dr Kirkham’s great experience and attention to detail help to minimise the risk of nerve injury, as he always prioritises patient safety and precise placement of the implants. He utilises high-quality implants and closely monitors their performance to detect any signs of loosening or failure early on.
Additionally, Dr Kirkham closely monitors the recovery process to identify and address any issues promptly. He provides comprehensive aftercare instructions and guidelines to help patients manage potential complications and optimise their recovery. Complications are rare, and by closely following these instructions, attending scheduled follow-up appointments, and communicating any concerns, patients can ensure early intervention and effective management of complications, should they arise.
Are You Concerned About Shoulder Arthritis?
If you’re concerned about shoulder arthritis, it’s crucial to understand the relationship between this condition, potential arthroplasty surgeries available, and the risk of dislocations. Shoulder arthritis can lead to joint instability and compromised shoulder function, increasing the likelihood of dislocations. However, arthroplasty offers a solution by replacing the damaged joint with an artificial one, restoring stability and reducing the risk of dislocations.
Dr Kirkham’s extensive expertise in preventing and managing shoulder dislocations post arthroplasty ensures optimal outcomes for his patients. With his years of delivering specialised care and his intimate knowledge of shoulder joints, he implements surgical techniques with precision and develops effective post-operative care strategies that promote long-term shoulder stability. By addressing individual factors and tailoring treatment plans, Dr Kirkham provides personalised care to minimise the risk of dislocations and maximise the functional benefits of arthroplasty.
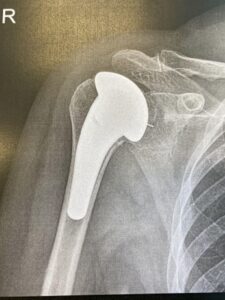
Figure 2 – X-Ray of shoulder following Arthroplasty
If you’re experiencing symptoms of shoulder arthritis, such as persistent pain, stiffness, and limited range of motion, it’s important not to ignore them. Seeking treatment early can prevent further joint damage and potential complications. Dr Kirkham and his team at the Sydney Orthopaedic Surgeon Clinic are dedicated to providing compassionate and effective care, and they have great experience in assisting individuals with shoulder arthritis.
Don’t hesitate to reach out and schedule a consultation if you’re experiencing symptoms. With early intervention and appropriate treatment, you can alleviate the pain you face, restore shoulder function, and regain the quality of life you deserve. Take the first step towards a pain-free and active future by seeking treatment today.
FAQs
1. How long does the recovery process take after shoulder arthroplasty?
Recovery time can vary depending on several factors, including the extent of the surgery, individual healing ability, and adherence to rehabilitation protocols. Typically, it takes several months to achieve significant improvement in shoulder function. However, it’s important to note that complete recovery and optimal results may take up to a year or more.
2. Can arthroplasty completely eliminate shoulder arthritis symptoms?
Arthroplasty is designed to alleviate pain, improve mobility, and enhance shoulder function. While it can provide significant relief from arthritis symptoms, complete elimination of symptoms is not guaranteed for everyone. The extent of symptom relief and overall outcomes can vary depending on individual factors, such as the severity of arthritis and adherence to post-operative care and rehabilitation.
3. Are there any long-term restrictions or limitations after shoulder arthroplasty?
In most cases, individuals who have undergone successful shoulder arthroplasty can resume their regular activities and enjoy an active lifestyle. However, it’s important to follow the specific guidelines provided by your surgeon. Heavy lifting or high-impact activities may need to be modified or avoided, as they can potentially put excessive strain on the shoulder joint. Consulting with Dr Kirkham will ensure you have a clear understanding of any necessary precautions.
4. Can shoulder arthroplasty be performed on both shoulders simultaneously?
Simultaneous bilateral shoulder arthroplasty, where both shoulders are operated on during the same procedure, can be considered in certain cases. However, the decision depends on various factors, including the patient’s overall health, surgical risks, and the surgeon’s recommendation. It’s important to have a thorough discussion with your orthopaedic surgeon to determine the best approach for your specific situation.
5. Can physical therapy be beneficial for shoulder arthritis without surgery?
Physical therapy can play a significant role in managing shoulder arthritis, even without surgery. A skilled physical therapist can develop an individualised exercise program to improve the range of motion, strengthen the muscles around the shoulder, and enhance joint stability. Physical therapy can also help alleviate pain, improve functional abilities, and delay the need for surgical intervention. It’s advisable to consult with a healthcare professional to determine the most appropriate treatment plan for your specific condition.
References
- Ortho Info (Shoulder Joint Replacement)
- Health Direct (Total Shoulder Replacement)
- Mayo Clinic (Shoulder Replacement Surgery)
- Ortho Info (Arthritis of the Shoulder)
- John Hopkins Medicine (Shoulder Arthritis)


