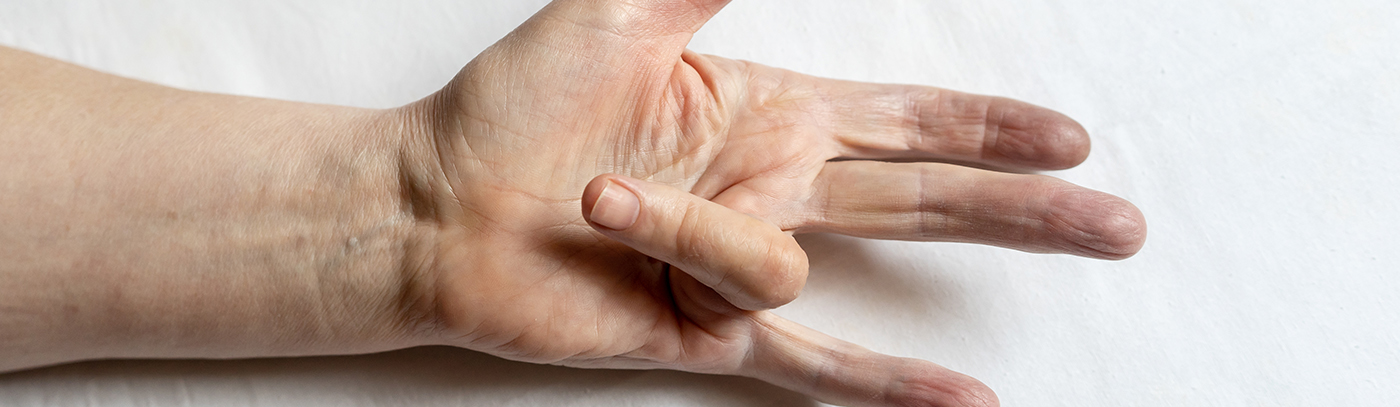
If you’ve noticed any thickening or tightening of the tissue in your hand, you may be experiencing Dupuytren’s Contracture. This common condition can cause your fingers to curl towards your palm, making it difficult to carry out everyday tasks. While this is not a life-threatening condition, it can have a significant impact on your quality of life.
Fortunately, at the Sydney Orthopaedic Surgeon Clinic, we specialise in the diagnosis and treatment of Dupuytren’s Contracture. Our team of medical professionals, led by Dr Stuart Kirkham, is dedicated to providing effective and personalised care to every patient. From non-surgical treatments like splinting and steroid injections to advanced surgical techniques of needle aponeurotomy , fasciotomy , fasciectomy and dermofasciectomy, a range of options are available to help relieve your symptoms and improve your hand function.
Whether you’re experiencing mild discomfort or more severe pain and limited hand mobility, the Sydney Orthopaedic Surgeon Clinic is here to help. Don’t hesitate to contact our friendly team to schedule a consultation with Dr Stuart Kirkham, who will work with you to find the best solution for your unique situation. Let’s work together to get you back to doing the things you love.
Anatomy Related To Dupuytren’s Contracture
To come to terms with Dupuytren’s Contracture, it’s important to first develop a sound understanding of the basic anatomy of the hand. The hand is a complex and intricate structure that is made up of bones, tendons, ligaments, muscles, and nerves, and each of these structures plays an important role in ensuring the hand can function.
The hand is comprised of 27 bones, of which there are 8 small carpal bones and 5 metacarpal bones that connect the wrist to the fingers, while 14 phalanges make up the fingers. Tendons are also present in the hand, and they are the strong fibrous cords that connect muscles to bones.
Several tendons are also within the hand, and they are responsible for controlling the movement of the fingers and thumb. Ligaments also form an important part of the hand’s anatomy, and they are strong bands of connective tissue that hold bones together to provide stability to the joints.
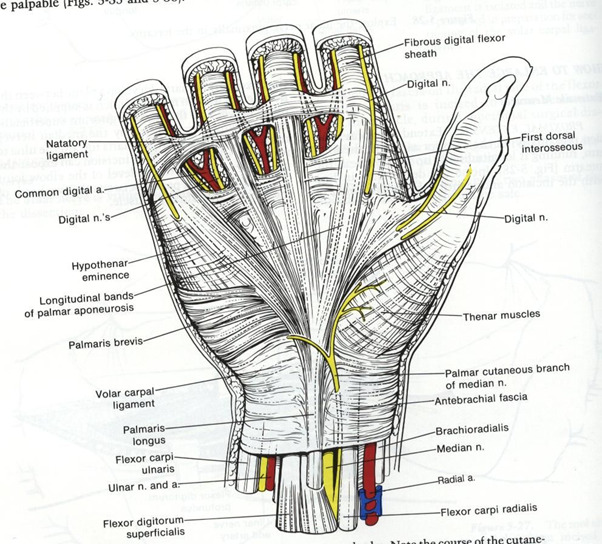
Ligaments also play a vital role in helping to keep the bones of the hand in place.
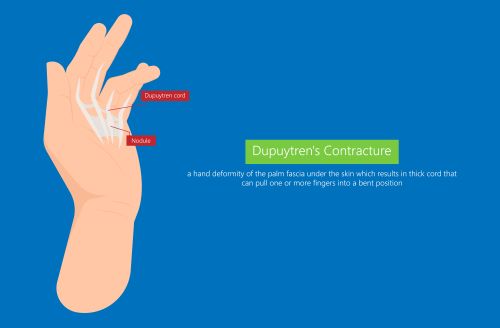
Dupuytren’s Contracture occurs when the palmar fascia, a layer of tissue that lies just beneath the skin on the palm of the hand, thickens and tightens over time. This can cause the fingers to slowly and progressively curl towards the palm, which ultimately limits the mobility of the hand. As the condition progresses, it can become increasingly difficult to perform simple tasks like shaking hands or grasping objects, particularly from within trouser pockets.
The palmar fascia is a network of connective tissue that helps to keep the skin on the palm of the hand in place. When this tissue thickens and shortens, it can cause nodules to form in the hand. These nodules can develop into cords of tissue that run from the palm of the hand to the fingers. As these cords thicken, they can cause the fingers to become permanently bent, leading to the characteristic finger contracture of Dupuytren’s Contracture.
Causes and Risk Factors of Dupuytren’s Contracture
Unfortunately, the exact cause of Dupuytren’s Contracture is not yet fully understood, but there are several factors that have been identified as increasing the risk of developing the condition. These factors can be broadly categorised as genetic, lifestyle, and medical factors that contribute to the onset of the condition.
One of the most significant risk factors for Dupuytren’s Contracture is simply a genetic predisposition. The condition is known to run in families, with those who have a family history of the condition being at a higher risk of developing it themselves. Studies have shown that at least 60% of cases of Dupuytren’s Contracture have a genetic influence.
Dupuytren’s Contracture has also been found more commonly in men than women. In particular, men over the age of 50 are at the highest risk of developing the condition. Nevertheless, women can still develop the condition, and they are most at risk after menopause.
While hereditary factors are often a significant influence, several lifestyle factors have also been identified as increasing the risk of developing Dupuytren’s Contracture. Smoking is one of the most significant risk factors, with smokers being up to three times more likely to develop the condition than non-smokers. Alcohol consumption has also been linked to an increased risk of Dupuytren’s Contracture, with heavy drinkers being at a greater risk of developing the condition than moderate or light drinkers.
Beyond genetic and lifestyle influences, a number of medical conditions have been linked to a greater risk of developing Dupuytren’s Contracture. Diabetes is one of the most significant, because individuals with the condition have been found to be up to three times more likely to develop Dupuytren’s Contracture when compared to those without diabetes. Epilepsy has also been identified as a risk factor, as those who have epilepsy are at a slightly higher risk of developing the condition.

Even though there is no guaranteed way to prevent Dupuytren’s Contracture from developing, understanding the risk factors and seeking treatment early can help to manage the condition effectively. However, if you have been experiencing the symptoms of Dupuytren’s Contracture, such as nodules or finger contracture, or if you have a family history of the condition, it’s important to seek expert medical advice as early as possible.
Dr Stuart Kirkham at Sydney Orthopaedic Surgeon Clinic has over 25 years of experience in treating and diagnosing the condition, and he is dedicated to providing the highest standard of personalised. His expert guidance can help you identify the condition before symptoms worsen, allowing you to steer clear of any inhibiting symptoms that may influence your daily life. Dr Kirkham was prestigiously invited by the French hand surgery society to present talks on Dupuytren’s to the French surgeons in France.
Symptoms and Identification of Dupuytren’s Contracture
Dupuytren’s Contracture is a progressive condition that typically develops slowly and over a number of years. While the early signs of the condition can be mild and easily overlooked, it’s important to seek medical attention as soon as possible to ensure the best possible outcome.
One of the earliest signs of Dupuytren’s Contracture is the development of small, painless nodules or lumps in the palm of the hand. These nodules can feel firm or rubbery, and they may be located near the base of the fingers or in the crease of the palm. Another early sign is pitting, which occurs when the skin over the nodules appears to be dented or even sunken.
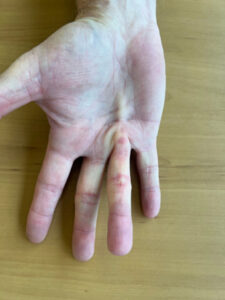
As Dupuytren’s Contracture progresses, the nodules can develop into thickened cords of tissue, and these typically run from the palm of the hand across to the fingers. These cords can cause the fingers to become bent towards the palm, and this can make it significantly more difficult to perform simple everyday tasks. In the most severe cases, the condition can cause a permanent loss of hand function.
If you have been or are continuing to experience any of these symptoms, or a member of your family has previously been diagnosed with the condition, it’s highly recommended that you consult a specialist with the relevant medical knowledge. At the Sydney Orthopaedic Surgeon Clinic, Dr Stuart Kirkham has been providing individualised and highly effective treatment options for Dupuytren’s Contracture for over 25 years. His vast medical expertise and personalised advice and treatment can go some way to delivering you the best possible outcome and improve your quality of life.
Diagnosis of Dupuytren’s Contracture
Diagnosing Dupuytren’s Contracture is essential in ensuring the most effective treatment plans are devised to manage the condition in an efficient manner. A thorough diagnosis typically involves a combination of verification activities, and this may include a physical examination, a series of questions regarding the patient’s medical history, and, in some cases, imaging tests.
During a physical examination, a doctor will carefully examine the affected hand for signs of Dupuytren’s Contracture, looking for the tell-tale nodules, thickened cords, and any signs of finger contracture. They may also assess the individual’s hand function and the range of motion that they have, as they will allow them to determine the extent and severity of the condition. Additionally, they will examine the other hand to compare it with the affected one to assess the degree of the deformity, if necessary.

A patient’s medical history is crucial in understanding the development and progression of Dupuytren’s Contracture. A doctor may ask about any family history of the condition, previous surgeries, lifestyle factors such as smoking and alcohol consumption, and any other medical conditions that may be contributing to the condition. Understanding these factors can help the doctor to determine the most appropriate treatment plan that is tailored to their specific requirements and is sensitive to any underlying conditions.
In some cases, imaging tests such as X-rays or MRI scans may be necessary to confirm a diagnosis of Dupuytren’s Contracture. These tests can help to visualise the extent of coexisting conditions, including arthritis, and provide valuable information for treatment planning. For instance, an ultrasound can help assess the potential for coexisting cysts, triggering digits and intermittent tendon entrapments, which might change the treatment in some cases.

If you’re worried that you may be experiencing the symptoms of Dupuytren’s Contracture, or you have a family history of the condition, it’s important to seek expert medical advice for a thorough diagnosis. Dr Stuart Kirkham and the team at the Sydney Orthopaedic Surgeon Clinic have years of experience in diagnosing and treating Dupuytren’s Contracture. By seeking their specialist care and advice, kickstarted by a thorough diagnosis, you can take the first step towards effective treatment and getting your hand health back on track. Don’t hesitate to contact our friendly team to schedule a consultation.
Treatment For Dupuytren’s Contracture
The approach to treatment for Dupuytren’s Contracture depends on the severity of the condition and the degree of finger contracture. While there is no guaranteed cure for the condition, there are several treatment options available that can help to manage the symptoms and improve the overall hand function in the short and long term.
Non-surgical treatments are typically the first port of call for Dupuytren’s Contracture, particularly in cases where the condition is mild or still in the early stages. These treatments may include splinting, which involves wearing a brace or splint to keep the affected finger in a straightened position, or steroid injections, which can help to reduce inflammation and improve finger mobility.
Another non-surgical option in the USA is enzyme injections, which involve injecting an enzyme into the affected tissue to break down the thickened cords and improve hand function.
Unfortunately, the collagenase enzyme treatment was removed from the Australian market about 3 or 4 years ago. There were a significant number of complications with respect to normal tendons; as well as a recurrence rate which was reported as high as 47% 2 years after treatment. These unfavourable outcomes and complications from Collagenase enzymne treatments led to the TGA in Canberra, Australia withdrawing collagenase as a treatment option in approximately 2018.
However, in more advanced cases of Dupuytren’s Contracture, surgical treatment may be necessary. These surgical treatments include needle aponeurotomy, a minimally invasive procedure that involves puncturing the skin with a needle to break up the thickened cords, or a fasciectomy, which involves removing the affected tissue to improve finger mobility. In more severe cases, a dermafasciectomy may be required, which involves removing the affected skin and underlying tissue and then replacing it with a skin graft.
Dr Stuart Kirkham and the team of experts at the Sydney Orthopaedic Surgeon Clinic have been delivered highly effective and individualised treatment options for many years, ensuring each patient receives a high standard of care to resolve their individual case of Dupuytren’s Contracture. From conservative non-surgical approaches to expertly conducted surgical procedures, Dr Stuart Kirkham always tailors his to each patient’s unique needs and circumstances. With years of experience and a commitment to staying up-to-date with the latest treatments and techniques, he is dedicated to providing the best possible care for each patient.
Prevention of Dupuytren’s Disease
While Dupuytren’s Contracture is a complex condition that can, unfortunately, be influenced by an individual’s genetic make up, there are steps that can be actively taken to reduce the risk of developing the condition and slow its progression.
Certain lifestyle factors such as smoking and excessive alcohol consumption have been linked to an increased risk of Dupuytren’s Contracture. By reducing these risk factors, individuals may be able to lower their risk of developing the condition or slow the rate that the condition progresses at.
Early intervention is key in managing Dupuytren’s Contracture and preventing its progression. If you notice any early signs of the condition, such as nodules or thickened cords, it’s important to seek medical advice promptly to prevent the condition from worsening.
Regular hand exercises can also be conducted, as they will help to maintain hand function and mobility and limit the influence of Dupuytren’s Contracture. These exercises may include stretching, gripping exercises, and other exercises recommended by a healthcare professional.
By taking steps to manage risk factors, seeking early intervention, and engaging in regular hand exercises, individuals can reduce their risk of developing Dupuytren’s Contracture or slow its progression. However, if you are experiencing symptoms of the condition or have a family history of the condition, it’s recommended that you contact Dr Stuart Kirkham and the team at the Sydney Orthopaedic Surgeon Clinic for a personal consultation.
With a comprehensive approach to treatment and a commitment to personalised care, we can help you to manage the symptoms of Dupuytren’s Contracture and improve hand function. Don’t hesitate to contact us to schedule a consultation.
Recovery From Dupuytren’s Contracture
Effective treatment for Dupuytren’s Contracture can help to improve hand function and relieve symptoms, but the time required for a full recovery can vary depending on the severity of the condition and the type of treatment the individual receives. After treatment, it’s important to follow a comprehensive post-treatment care plan to ensure optimal recovery.
After undergoing a surgery or completing non-surgical treatment for Dupuytren’s Contracture, Dr Kirkham provides all patients with a personalised post-treatment care plan to follow that promotes healing and prevents complications from occurring. This may include ensuring the hand remains elevated, changing dressings regularly, and avoiding strenuous activities until advised by a healthcare professional.

Rehabilitation and physiotherapy can also play a crucial role in the recovery process for Dupuytren’s Contracture. A physical therapist or hand therapist can work with the patient to develop a rehabilitation program that includes exercises to improve hand function and mobility. They may also use a wide variety of techniques to reduce any pain and swelling the patient is experiening, such as a massage or ultrasound therapy.
Ultimately though, the recovery timeline an individual faces when dealing with Dupuytren’s Contracture will depend upon the severity of their condition and type of treatment they received. Non-surgical treatments such as steroid injections or splinting typically have a shorter recovery time, with patients typically returning to normal activities within a few weeks. Surgical treatments may however have a longer recovery time, with patients requiring several weeks of rest and rehabilitation before returning to normal activities.

At the Sydney Orthopaedic Surgeon Clinic, Dr Stuart Kirkham and our team of experts are dedicated to providing comprehensive post-treatment care and rehabilitation to help patients achieve the best possible outcomes. We work closely with each patient to develop a tailored care plan that meets their individual needs and circumstances.
Complications If Dupuytren’s Contracture Is Left Untreated
While Dupuytren’s Contracture may seem like a minor inconvenience, it can have serious consequences if it is left untreated. Without proper treatment, the condition can progress and lead to a range of complications that can impact the individual’s hand function and their quality of life.
One of the most significant complications of untreated Dupuytren’s Contracture is permanent finger contracture, where the fingers become permanently bent or curved. This can make it difficult or even impossible to perform everyday tasks like holding objects, writing, or typing.
Dupuytren’s Contracture can also lead to a loss of hand function, making it difficult or impossible to perform everyday tasks. This can impact a person’s ability to work, engage in hobbies or activities, or perform basic self-care tasks.
In addition to physical complications, Dupuytren’s Contracture can cause pain and discomfort, which can have a significant impact on quality of life. This pain can be persistent and can make it difficult to perform everyday tasks.
The impact of Dupuytren’s Contracture may also extend beyond physical symptoms. When the condition persistently impacts an individual, it has been found to have adverse psychological impact on patients, with feelings of anxiety, depression, and isolation being common among those with the condition, particularly if they are experiencing significant physical limitations.
At the Sydney Orthopaedic Surgeon Clinic, we understand the potential complications that can arise from untreated Dupuytren’s Contracture, and Dr Stuart Kirkham is committed to providing effective and timely treatment that prevents these complications from occurring. By seeking timely treatment, you can avoid these potentially serious complications and get your hand health back on track.
Don’t Let Dupuytren’s Contracture Grip Control Of Your Life

Dupuytren’s Contracture is a condition that can significantly impact hand function and quality of life if left untreated. However, with the right treatment approach, it’s possible to manage symptoms, improve hand function, and prevent complications.
At the Sydney Orthopaedic Surgeon Clinic, Dr Stuart Kirkham and our team of experts are dedicated to providing comprehensive and effective treatment options for Dupuytren’s Contracture. From non-surgical treatments like splinting and injections to advanced surgical techniques like needle aponeurotomy and fasciectomy, we offer a range of options to help relieve symptoms and improve hand function.
Early diagnosis and intervention are crucial in managing Dupuytren’s Contracture and preventing complications. If you’re concerned that you may be suffering from Dupuytren’s Contracture, don’t hesitate to contact our friendly team to schedule a consultation with Dr Stuart Kirkham. Our team can provide a thorough evaluation and develop a personalised treatment plan tailored to your individual needs and goals.
By seeking timely treatment and following a comprehensive post-treatment care plan, you can prevent complications and achieve optimal hand health. Contact the Sydney Orthopaedic Surgeon Clinic today to take the first step towards effective treatment and improved quality of life.
FAQs
1. How long does it take for Dupuytren’s Contracture to progress?
The progression of Dupuytren’s Contracture can vary greatly from person to person. Some individuals may experience slow progression over several years, while others may experience more rapid progression. It will depend on gene expression ie the chromosome that you have inherited on your DNA. The condition typically starts with small nodules or pits on the palm, which can gradually progress to form thick cords and contracture of the fingers. Early diagnosis and intervention can help prevent the condition from progressing and causing complications, so it’s important to seek medical attention if you’re experiencing any symptoms.
2. What are the potential complications of Dupuytren’s Contracture surgery?
Dupuytren’s Contracture surgery is generally safe and effective, but like any surgical procedure, it carries some risks. Complications can include recurrence of cords, infection, bleeding, nerve damage, and stiffness in the hand. However, these complications are rare and can often be prevented through proper post-operative care and rehabilitation. However, you can rest assured that Dr Kirkham will always discuss the potential risks and benefits of surgery with you before any surgical treatment is conducted, and these risks can be further minimised by carefully following all post-operative instructions.
3. How long does recovery take after Dupuytren’s Contracture surgery?
Recovery time after Dupuytren’s Contracture surgery can vary depending on the type and extent of the surgery performed. In general, patients can expect to wear a splint for several weeks and participate in rehabilitation exercises to regain hand function. However, in the most severe cases, full recovery can take several months. Dr Stuart Kirkham will provide specific instructions on the post-operative care and rehabilitation necessary for your case, and this can help speed up the recovery process and improve outcomes.
4. Can Dupuytren’s Contracture recur after surgery?
While Dupuytren’s Contracture surgery can be effective in improving hand function and preventing the condition from progressing, there is a small risk of recurrence. The risk of recurrence can be minimised through proper post-operative care and regular follow-up appointments with a healthcare provider. If you experience any symptoms after surgery, it’s important to seek medical attention promptly to prevent recurrence or complications.
5. Is Dupuytren’s Contracture hereditary?
There is evidence to suggest that Dupuytren’s Contracture can be hereditary, meaning that it can run in families. While the exact genetic cause of the condition is not fully understood, research suggests that certain genetic mutations may increase the risk of developing Dupuytren’s Contracture. However, other factors such as age, gender, lifestyle, and medical conditions can also contribute to the development and progression of the condition. If you have a family history of Dupuytren’s Contracture or are experiencing any symptoms, it’s important to seek medical attention for early diagnosis and treatment.
6. What happens if Dupuytren’s Contracture is left untreated?
If Dupuytren’s Contracture is left untreated, the condition may progress, causing the affected fingers to gradually contract and bend towards the palm. This can lead to functional limitations, making it challenging to perform everyday tasks. Severe cases may result in a permanent deformity that hinders hand movement. Early diagnosis and appropriate treatment by a hand specialist like Dr. Stuart Kirkham can help prevent further progression and improve outcomes.
7. What are the warning signs of Dupuytren’s Contracture?
Warning signs of Dupuytren’s Contracture include the development of small, painless nodules or lumps in the palm, usually near the base of the fingers. As the condition worsens over time, thick cords or bands may form in the area, leading to the fingers gradually bending inward. Reduced finger extension, difficulty placing the hand flat on a surface, and the formation of pits or grooves on the skin of the palm are other potential warning signs. If you notice any of these symptoms, be sure to consult Dr Kirkham for an evaluation of your condition adn the development of a personalised treatment plan.
8. Is Dupuytren’s Contracture a form of arthritis?
Dupuytren’s Contracture is a form of arthritis that affects the connective tissue in the palm and fingers, leading to the formation of nodules and cords that cause the fingers to bend inward. While both Dupuytren’s Contracture and arthritis can affect hand function, they have different underlying causes and require different treatment approaches. A hand specialist like Dr. Stuart Kirkham can accurately diagnose and provide appropriate treatment for Dupuytren’s Contracture.
References
- Ortho Info (Dupuytren’s Disease)
- Mayo Clinic (Dupuytren’s Contraction)
- American Society For Surgery of The Hand (Dupuytren’s Contracture)
- Better Health Channel (Dupuytren’s Contracture)
- Health Direct (Dupuytren’s Contracture)